The fight against pediatric brain tumors
Written by Stephanie Stursberg
20. December 2021
Childhood brain tumors are thankfully rare, but are often associated with poor prognoses and low survival rates. Despite the progress in this field over recent years, the lack of funding for research has meant that the potential breakthroughs to help fight this orphan disease have not always been possible. INTEGRA is proud to support the important work being conducted by the DIPG Fighter research group at the Ludwig Maximilian University of Munich (LMU) with a festive donation of 20,000 EUR. We had the opportunity to speak to Dr Alexander Beck about his group’s groundbreaking research, and how the funds will help push their findings into the clinic.
Table of contents
How did you get into pediatric brain tumor research, and what does your research involve?
Prior to setting up the DIPG Fighter lab, I worked as a fellow in pediatric neuro-oncology in Boston, USA, which is what inspired me to be truly dedicated to the translation of research towards the development of drugs to treat this pediatric brain tumor. Our group looks at diffuse intrinsic ponsglioma (DIPG), which is a rare form of brain tumor usually affecting children between five and nine years of age, and currently with no significant long-term survival beyond five years.
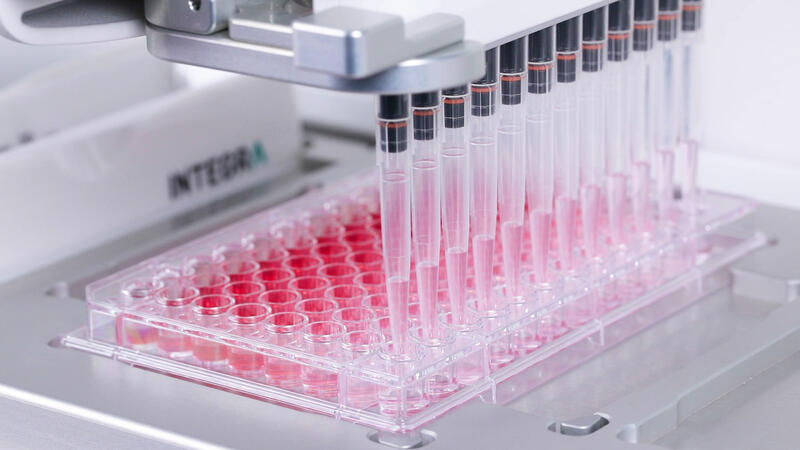
Our focus is to rebuild sophisticated preclinical models to identify drugs that will eventually go into the clinic. Much of our work involves studying drug efficacy, blood-brain barrier (BBB) penetration and toxicity, as well as the biology of the tumor itself. We use a range of tumor models – preclinical patient biopsy samples and brain organoid cultures – that are biologically similar to DIPG, as well as BBB models to assess the drug permeability, and techniques to understand dose-limiting toxicities.

Has there been any progress?
We have recently had success with one drug called ONC201, which has gone into the clinic after a single agent trial. We have shown some short-term survival benefits, extending the life span of children with DIPG by approximately two years but, unfortunately, it doesn't seem to rescue anybody in the long term.
However, even this limited success has been very motivating for us, because we have never seen anything work like this before. We have now identified three drugs – one of which is ONC201 – to use in combination trials, to see if this approach can further improve outcomes.
Are there any new drugs you're now looking at, or is it a continuation of research based on ONC201?
We’re still in the early stages of research with DIPG but, as one drug isn’t going to cut it, our focus is to build on ONC201 to discover new drugs that can be used in a sequential treatment protocol. Although we can give ONC201 to patients, some malignant tumor cells may survive and eventually become resistant to it, therefore a second drug that is effective on the remaining tumor population will be required. The difficulty is that when the treatment is stopped, or even if we continue it, the tumor may return.
We are currently studying resistance mechanisms and examining the extent of reduction in the tumor after exposing them to a drug regimen that is comparable to what a child would get in the clinic. We are hopeful of this approach as it has already been shown to be effective for treating various diseases. If you take leukemia, for example, 95 % of children with the cancer are cured following a two-year detailed plan, which involves administering around 20 drugs that work tremendously well.
How do you select the next drug after the tumor cells become resistant to the first drug?
Our aim is to get this into the clinic fast, so we don't want to spend one or two years finding out the exact mechanism. This is why we have some prerequisites when it comes to identifying suitable compounds. One of the requirements is that there must be Phase I clinical data – such as a toxicity profile – to determine if the drug can be safely taken by humans.
The second is that the drug we’re looking to repurpose needs to be approved and available on the market for any condition. Nobody knows if the tumor cells will become resistant to drugs similar in structure to ONC201, which is why we cannot afford to exclude any from testing as it may have a different mode of action. The mouse model has been the best in the field so far, but it has not been feasible to conduct accurate, high throughput screening of 1,000 compounds for DIPG.
As we cannot spend time testing every available drug for DIPG treatment, we’ve introduced a target identification step that looks at biomarkers of molecular structures or predetermined moieties. Pathways in the tumor cells that we know are likely to be active are identified, allowing us to only test a selected panel of drugs targeting those routes. We can still narrow down these tested drugs to one or two that are most preferential for the patient. However, if we find just one pathway to be active, there might still be 50 drugs available to potentially treat the patient.
We prioritize by looking at the additional layers of information, including BBB penetration and toxicity profiles. The insurance company makes the final decision – whether they will cover the cost of the selected drug – after negotiations that can take up to six months. The main concern is the availability of the drug for the predicted time of treatment, which is only about four or five weeks after the initial surgery.
Are there any major developments in your research? Do you think personalized medicine could be the way forward to tackle DIPG?
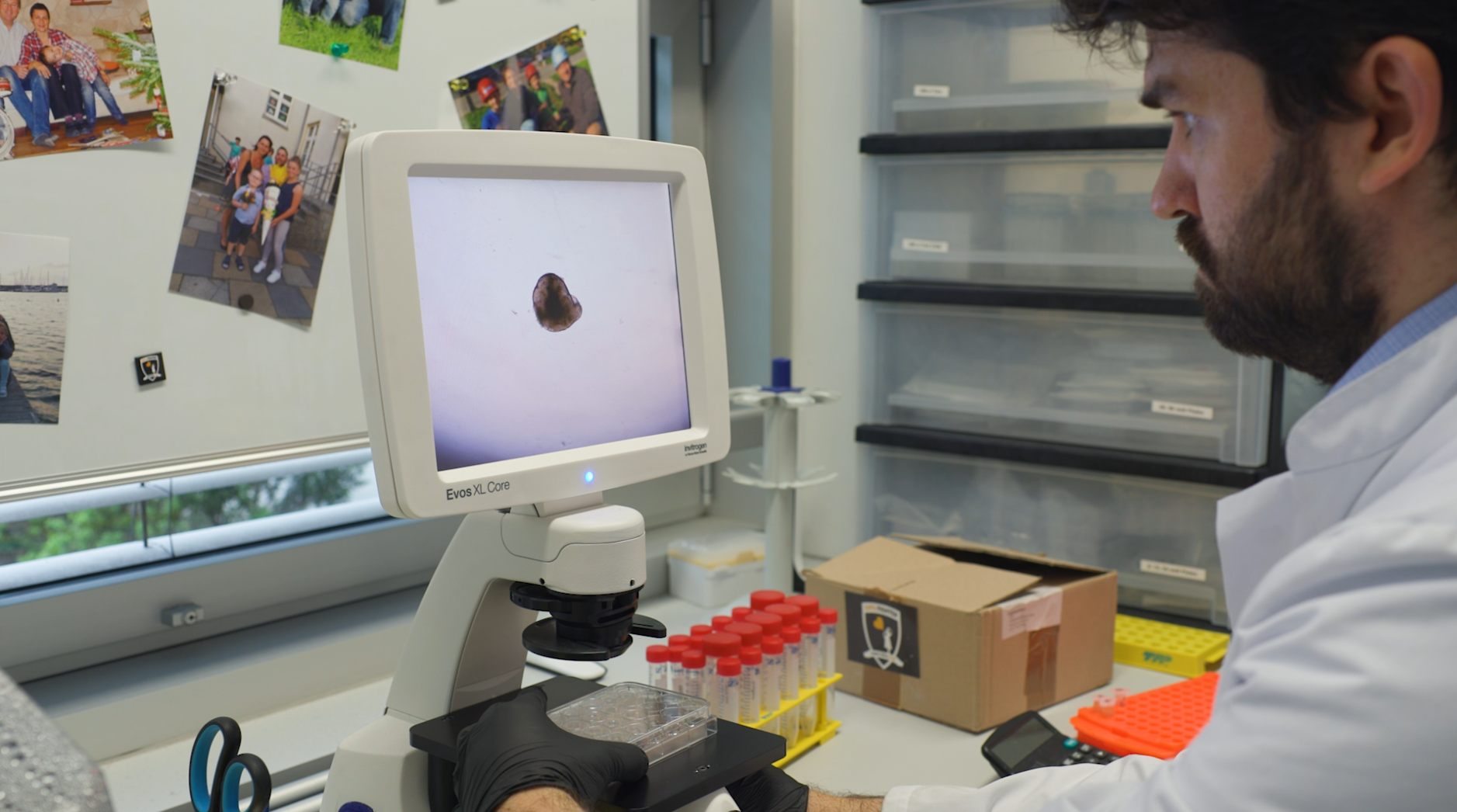
What we’re finding is that tumors are heterogeneous, meaning that they have really variable compositions and might respond very differently to a drug. We're trying to move towards a personalized approach by building models that use brain organoid cultures to give accurate predictions of what happens in the clinic. Personalized medicine is relatively new, and a lot of researchers and clinicians around the world use it to treat different types of cancers.
Assessing the outcome of a personalized medicine is very different to a clinical trial in which there are two groups of subjects, for example, one taking the drug and the other taking a placebo. Typically, when there’s just one patient receiving a drug, there is insufficient evidence to show that they might benefit from it and no comparison to show whether the patient is better off without the drug.
Personalized medicine for orphan diseases like DIPG – that have no standard of care – is generally much harder to get approved and requires a lot of effort negotiating with insurance companies. We know that without any treatment, most of the kids would only live a couple of weeks after diagnosis, so getting approval could literally be a matter of life or death for somebody.
Unfortunately, radiation therapy and chemotherapy offered to a patient, in the meantime, will significantly change the brain tumor, leading to our initial prediction of a personalized medicine not being suitable for that individual.
We have already used this strategy for a more common entity, glioblastoma – another very devastating brain tumor – for which we have many more patients and tissue to work with, and this actually works quite well. For DIPG, the way we start is by removing a small number of tumor tissues from an individual patient’s brainstem, growing cultures from them, testing drugs directly on these cells, and then reporting to the clinicians about what our treatment recommendation is for that individual.
I am confident that there will be better tools in the future to ensure rapid approval, or even preapproval, after informed personalized testing. This field is moving really fast, and I believe that we are making steps in the right direction in a process that will hopefully improve over time with advanced technologies.

How will INTEGRA’s festive donation help?
We are very pleased to have been chosen to receive this year’s festive donation of 20,000 EUR from INTEGRA. Although our team is very determined, and we have an excellent infrastructure here at LMU, progress in this area is very difficult; we don’t always have the vital funds to further our findings, which is why this donation is much appreciated.
It will fund the continuation of our existing cutting-edge research projects, allowing us to purchase all the consumables, cell culture plates and media necessary to further develop our organoids and tumor cell models. In the next five years, there will be particular emphasis on preclinical drug screening and testing, with the ultimate goal of identifying approved therapeutics that can be repurposed for new clinical applications.
To find out more about the DIPG Fighter lab’s work, visit www.dipgfighter.com/research.